Nafissa Ikerodah is both a detective and diplomat of sorts. On a Saturday morning in early March, the Disease Surveillance Officer in Edo State area rushes to a household where a man has just died of Lassa fever.
The young father left behind two sons who show symptoms of the infectious disease. Nafissa wants to get the children to a hospital as quickly as possible. One boy is so weak he can barely stand.
She must also identify all the people who recently came into physical contact with the deceased father so they can be monitored for signs of the viral haemorrhagic fever.
Both jobs are difficult in a community reeling from a recent death and fear for their own lives.
“The first time you visit and tell them you are a disease surveillance officer, they are always scared,” says Nafissa.
Faith Ireye, the World Health Organisation’s (WHO) Edo State Coordinator, accompanies Nafissa. They arrange for an ambulance to pick up the boys and ask the family to provide the names of the deceased patients’ contacts within the community.
“Contact tracing is the bedrock of infectious disease outbreak control. If contact tracing is not done, people who come into contact with Lassa fever patients stay in their homes, become symptomatic, infect more people, and make the outbreak bigger and bigger,” says Faith.
Nafissa visits every identified contact of the deceased father. She records names, telephone numbers, and the date of their last encounter with the patient. She gives each a thermometer for personal temperature checks and arranges to call on the contacts daily for the next 21 days to note their temperature. If anyone is suspected of having Lassa fever, they will be taken to hospital for a confirmatory test and, if positive, provided with care in a special isolation unit.
By March 18, 3,675 contacts of the 376 confirmed Lassa fever cases in Nigeria had been identified and more than three-quarters had completed their 21 days of monitoring.
In Edo State – where the outbreak has been spreading particularly fast – WHO, the Nigeria Centre for Disease Control (NCDC), and the local government are reaching out to communities with a large-scale awareness raising campaign.
Sensitisation sessions will aim to reach nearly 9,000 community leaders, town announcers, headmasters, herbalists, healthcare workers, clinicians, church leaders, and women who work in local markets.
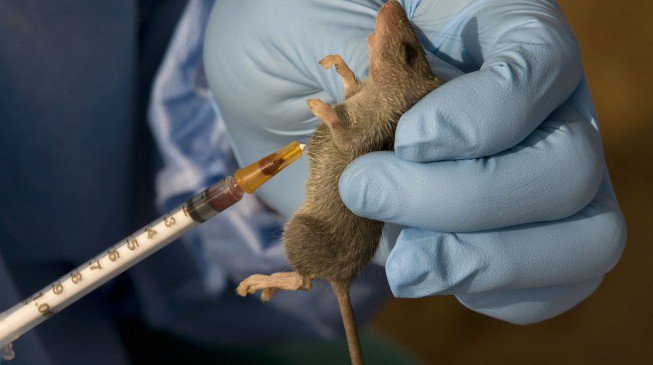
The Lassa virus is transmitted to humans mainly through handling infected rats, food or household items contaminated by the rats’ urine and faeces. The virus can spread between people through direct contact with the body fluids of a person infected with Lassa fever, as well as contaminated bedding and clothing.
Community members are being advised of a range of preventive measures including washing hands regularly, storing food in containers with lids, keeping their homes clean and tidy to discourage rats from entering and cooking foods thoroughly.
Garri, which is made from cassava tubers, is a staple food in this part of Nigeria. Traditionally, families have left the crushed cassava outside in the sun to dry out. During the sensitisation sessions, participants are encouraged to dry garri through frying over a hot stove, rather than in the sun.
After one awareness raising session, primary school teacher Mary Enaholo says she has learnt important hygiene lessons that she will share.
“I will take the information that I learnt today to my pupils so they will take these messages back to their homes,” she says.
But changing behaviours is no easy task.
In one house, Faith and her team find a basket full of rats being kept as pets by a boy. Nearby, garri is being dried in the sun. Faith quickly advises the household to cover the food.
The WHO says it is working with communities to deliver messages that will encourage preventive actions and ultimately save lives.
